Gabby Giffords Q&A with Dr. Chethan Sathya, Director of Northwell Health’s Center for Gun Violence Prevention
Gabby
Chethan, thank you for speaking with me today! It’s a pleasure to get to know you and your work better, as we fight for a country free from gun violence.
Chethan
Gabby, I sincerely thank you for sharing your perspective and taking the time for this conversation. You are an inspiration to us all in healthcare, and your advocacy and tireless efforts to help reduce gun violence motivate us to do whatever we can within the healthcare lane to help prevent firearm injuries.
As a trauma surgeon, I am all too often pulling bullets out of children and telling parents or loved ones that they’ve lost a family member to a largely preventable injury. But our job is easy compared to yours…We treat the bullet wound and try to save a life. And if we are successful, we don’t have to live with the devastating long term health effects of firearm injuries.
I’d love to hear about what the experience was like for you after your emergency surgery, I can only imagine how scary that must have been.
Were there particular moments that stood out to you during your hospital stay?
Gabby
I arrived at the hospital in critical condition. I don’t remember much from that time, but it wasn’t clear that I was going to make it, and it was a terrifying time for my loved ones. Every time I hear about a shooting—which is far, far too often—my heart goes out to all the loved ones of the people who were at that grocery store, or FedEx building, or school (no part of this nation is untouched by gun violence). It’s difficult for those who haven’t lived through it to understand the uncertainty, the frustration, and the trauma of those early days.
10 Years Ago, My Boss Nearly Lost Her Life
Peter Ambler—Jan 08, 2021
As I emerged from critical condition, I did my best to remain optimistic while embarking on my journey to regain the ability to speak and walk. Physical therapy, speech therapy, and music therapy all became parts of my daily life. One of my first big breakthroughs was bursting out into song, which happened before I formed my first full sentence. It wasn’t easy being hospitalized for so long. My husband Mark, my friends and family, my congressional colleagues, and the members of my care team stayed by my side kept me motivated. I’m still overcome with gratitude when I think about their unwavering support in those dark and difficult days.
Chethan
Your strength and discipline toward recovery is incredible. How do you stay motivated to move forward? What are some of the biggest struggles that you have faced throughout your years of active recovery? This is a perspective we rarely hear about in medicine, as we often treat the injury and then disconnect.
Gabby
Living with aphasia comes with its fair share of struggles. Speaking used to come easily for me, but now it’s hard to find the right words. I’ve made so much progress, thanks to my wonderful speech therapist, Fabi. When I first was relearning to speak, all I could say was “what, what, what,” and “chicken, chicken, chicken.” In 2020, I gave my longest speech since being shot at the Democratic National Convention.
I don’t let my aphasia keep me from pursuing my passions, big or small. When I’m not fighting for gun safety, I also ride my bike, take Spanish lessons, and play French horn. And while my aphasia doesn’t define who I am, you’re right—we rarely hear about the long, often lifelong struggles of those who have been shot and survived. It’s been a long journey these last 10 years, but I always try to stay optimistic. I’ve made gun violence prevention my life’s work, and this movement to save lives is a big part of what keeps me motivated.
Chethan
I firmly believe healthcare has the unique ability to approach gun violence prevention from an apolitical harm reduction standpoint, by focusing purely on firearm safety and violence prevention. From my standpoint, this has nothing to do with the Second Amendment or gun ownership. How can healthcare providers work with you and others to be successful in depolarizing this public health issue?
Gabby
This is a great question. Not everyone views gun violence as a public health issue, but healthcare providers can and should play a critical role in making the case for why it is. Nearly 40,000 Americans every year lose their lives to gun violence, and tens of thousands more are injured. We treated automobile deaths like a public health epidemic in the 60s and 70s, tackling the problem through a combination of research-based laws and safety reforms. As a result, car deaths declined. We shouldn’t treat gun violence any differently.
Healthcare providers can also destigmatize gun safety by having conversation with patients about things like safe storage, mental health, and overall well-being. We need everyone in this fight: Republicans, Democrats, gun owners, doctors, young people, CEOs. If we work together and make our voices heard, we can make lasting change and save lives from gun violence.
And now I want to turn the tables and ask you a few questions! As the director of Northwell Health Gun Violence Prevention Center, you’re playing a critical role in mobilizing the healthcare industry around the gun violence epidemic. Can you talk about why you see gun violence as a public health issue, and what role the healthcare industry should play in gun violence prevention?
Chethan
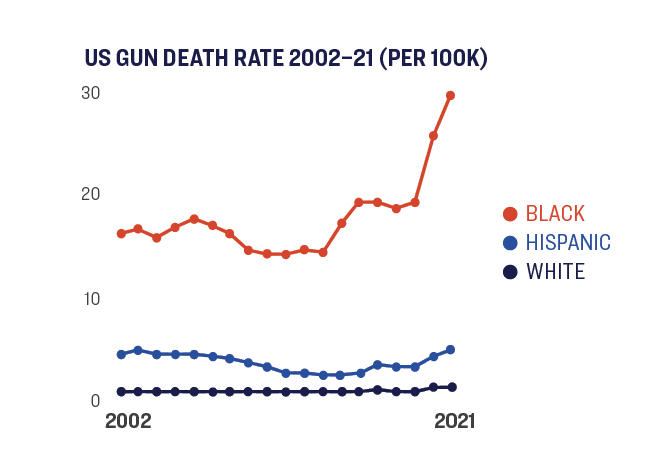
BLACK AMERICANS ARE AT HIGHER RISK OF GUN HOMICIDE
Source
Centers for Disease Control and Prevention, National Center for Health Statistics. Underlying Cause of Death 1999-2020 on CDC WONDER Online Database, released in 2021. Data are from the Multiple Cause of Death Files, 1999-2020, as compiled from data provided by the 57 vital statistics jurisdictions through the Vital Statistics Cooperative Program. Accessed at http://wonder.cdc.gov/ucd-icd10.html on Mar 17, 2022. Calculations were based on five years of the most recently available data: 2016 to 2020
Anything that’s killing upwards of 40,000 people a year is a public health issue, and should be treated as such. Gun violence is a leading cause of death for Americans and directly affects the health of our communities—that’s particularly true for communities of color. For young Black men in America, gun violence is the leading cause of death—more than the next nine causes combined. And the staggeringly high rates of firearm injuries we see in this country surpass many other health risk factors that we label “epidemics.” So this isn’t just an epidemic—it’s a preventable, uniquely American public health crisis.
I believe there is a crucial role for the healthcare industry to play in confronting gun violence. We have the unique ability to address this issue from an apolitical, harm reduction standpoint, purely focused on safety and injury prevention. I’m grateful to work for Northwell, where we have a real top-down commitment to gun violence prevention. In order to make the kind of change we so desperately need in this country, we need a similarly deep commitment across our entire industry.
The good news is, there’s precedent. The healthcare industry has risen to the challenge when it comes to tobacco, motor vehicle safety, and other issues that have been historically stigmatized the way gun violence is, like substance use disorders and HIV. We’re poised to do the same when it comes to gun violence. We can transcend politics, depolarize this issue, and implement strategies that are focused on well-being and safety. Because at the end of the day, our top priority will always be the safety and health of the families we serve.
Gabby
You’re a pediatric trauma surgeon with experience operating on children with gunshot wounds. Surgeons played a crucial role in my recovery after I was shot and I’m eternally grateful for the level of care you all provide your patients. How has your profession informed your advocacy for firearm injury prevention?
Chethan
I’m a Gun Owner and Pediatrician, and I’m Using my Voice to End Gun Violence
Claudia Fruin—Jun 10, 2021
First of all, I’m grateful for the care you received, and inspired by what I know amounts to years of tireless work on your part toward your recovery. I know I’m far from alone in putting you at the top of my list of heroes.
To answer your question, as a pediatric trauma surgeon, I see and treat children with bullet wounds. I pull bullets out of babies. I see the devastating long-term effects of gun-related disabilities.
It’s hard to describe what it’s like to watch a child die from a bleeding bullet wound. What’s worse is having to tell parents over and over again that they’ve lost a loved one to a preventable disease. I will forever be haunted by the faces of parents as they watch their child slip away in the trauma bay.
I can’t imagine doing what I do and not being passionate about this issue. Given these experiences, and inspired by survivors like you, I feel a responsibility to play at least a small part in the larger effort of preventing gun violence. Enough is enough.
Gabby
You were recently awarded a substantial research grant from the NIH to study gun violence prevention and implement a first-of-its-kind protocol to universally screen among those at risk of firearm injury. Our country has a dire need for more research into the causes of gun violence, so this is a tremendous step forward. What excites you most about this research opportunity?
Chethan
You’re absolutely right—the ability to research firearm injury prevention in itself is tremendously exciting. Gun violence is akin to a new disease: There is much more research to be done on prevention, and what we know with respect to preventative strategies is based on weak data. So I cannot overstate how important this much-needed federal funding for firearm injury prevention research is. Your efforts to advocate for this funding have really transformed and escalated healthcare’s involvement on this public health issue. So I want to thank you for that.
Research Roundup: An Analysis of Gun Violence Publication Trends in 2021
Alex Nguyen, Kelly Drane—Feb 08, 2022
The most exciting part of our research study, which is called “We Ask Everyone: Firearm Safety is a Health Issue,” is that we will be the first health system to universally screen all patients for firearm injury risk. Our study has nothing to do with gun control or ownership; it’s purely focused on injury prevention and harm reduction. By asking every single patient questions related to firearm injury prevention—the same way we counsel patients about sugar intake, exercise, or motor vehicle safety—we can normalize conversations about firearm safety between doctors and patients. This is a big deal, because right now, very few doctors talk to patients about this. We are hoping to change that by researching what prevents these conversations, and what enables them. I’m also excited that the voices of gun owners and community-based organizations, which are critical to our efforts, are integrated into this research.
The bottom line is this: If we can figure out how to destigmatize and depoliticize conversations around firearm injury prevention, it could have a far-reaching impact on other sectors as well, including corporations and policy makers.
Gabby
The federal landscape around gun safety is changing. The House passed universal background checks last year, and President Biden announced a series of executive actions on gun reform. How is this shaping your current work and future plans at Northwell?
Chethan
It’s a breath of fresh air. We feel empowered to take this on as a public health issue, and we are even more motivated to study and implement solutions to gun violence. Our focus is not on legislation—as I’ve said, we are approaching this from an apolitical standpoint—but having an administration that really sees gun violence as the public health issue it is goes a long way in making our research possible, and spurring us on.
Gabby
Lastly, what keeps you going in this long and difficult fight?
Chethan
I’m constantly inspired by survivors like you! As physicians, our job is easy compared to what you have gone through. So the simple answer is: Your strength in recovery drives us to want to do better in preventing these injuries. And your courageous advocacy has inspired many of us to stand with you.
Another thing that keeps me going is hope—hope that the world can be a safer place, that we can find common ground on an issue that continues to kill thousands of Americans from all walks of life.
Finally, it’s hard to overstate how energizing new research is. As we get more data, we are starting to see the real benefits of healthcare-based interventions to prevent firearm injury. Knowing we can make a difference plays a big part in motivating us to continue to explore this issue and advocate for our patients.
TAKE ACTION
The gun safety movement is on the march: Americans from different background are united in standing up for safer schools and communities. Join us to make your voice heard and power our next wave of victories.
GET INVOLVED